Services – Physiotherapy
What is Physiotherapy?
What is a Physiotherapist?
A Physiotherapistis a primary health care professional (you don’t need a doctor’s referral to see one), with a university degree, and is a registered physiotherapist with a College of Physiotherapists. They combine an in-depth knowledge of anatomy, physiology, pathology, and physical movement with their highly skilled hands on assessment and treatment techniques to assist a client in reducing pain, improving function, increasing strength and conditioning, and helping them to return activity.
Who would Benefit from Physiotherapy?
Physiotherapy can help people of all ages from children to seniors, for a large range of conditions and ailments. Whether you have a sports injury, are recovering from surgery, or you have an injury due to something in your daily life, it is important to have it assessed and treated properly. After an injury, pain will typically subside gradually, but it is often because we have learned to adapt our motion to avoid the pain, without being aware of it. This adapted movement can persist and often leads to further dysfunction, decreased mobility, and chronic pain which can be harder and take longer to treat in the future. Once the pain is gone it is essential to regain muscle activation, maximum mobility and strength to avoid future injury pain.
What to Expect from a Session
You will have a one on one session with the physiotherapist, where you will be assessed for movement, function, alignment, biomechanics, strength and specific injury. After your assessment the therapist will educate you on your diagnosis, prognosis, and discuss what treatment options are available. All treatments will be performed and monitored by your physiotherapist. Your therapist will give you exercises to perform on your own and educate you on activities you should and shouldn’t do.
Conditions Requiring Physiotherapy

Treatment Techniques
INTRAMUSCULAR STIMULATION (IMS)
Treats neuropathic pain, caused by a nerve irritation, often by a tight muscle
MANUAL THERAPY
Used to mobilize, manipulate joints and massage muscles to reduce pain and improve range of motion and function
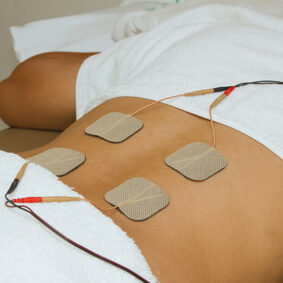
ELECTRICAL MODALITIES
Muscle stimulators, Interferential Current, TENS and Ultrasound use different sources of energy to treat injuries
THERMAL AGENTS
Heat – to reduce pain and reduce muscle tone. Ice – to reduce pain and control swelling.
THERAPEUTIC EXERCISES
Customized for each client to reactivate and strengthen inhibited and weakened muscles to regain balance, strength and conditioning.
ACUPUNCTURE
involves inserting thin needles into the body at specific points to provide pain relief and muscle relaxation
